
Via Danielle Page (@TheVeganPage) on Twitter
COW-MADE, MAN-MADE, OR MOTHER-MADE?
- Under the Microscope
- Moo Milk vs. Mom’s Milk
- Modern Formula vs. Human Milk
TOXINS IN INFANT FORMULA
**Also check out Part One (Why Isn’t Every Baby Breastfed?) and Part Three (Making a Baby-Friendly Culture Amid Formula Marketing) of this series.**
Cow-Made, Man-Made, or Mother-Made?
“Although most doctors avoid saying so, out of fear of alienating some clients, formula-fed babies are generally less healthy than breastfed babies. The cognitive development of babies fed formula doesn’t equal that of those who are breastfed. Breast milk protects against disease and promotes optimal brain growth. Formula does neither of these things.” – Kathleen Huggins, The Nursing Mother’s Guide to Weaning
There we go again: formula is not an equivalent substitute to breast milk, it’s just a good alternative. The only breast milk I’ve ever tasted is my own and I’ve been doing just fine (I think?) in my adult life as a previously formula-fed baby. So when I say a “good” alternative, I don’t secretly mean a “poisonous” one.
Here’s my caveat: I don’t recite the following information in attempt to kill the spirit of formula-feeders, to insinuate that modern infant formula is poison, or out of fear that the benefits of breastfeeding cannot stand on their own without reminding of the drawbacks of formula. This information should be understood by anyone raising a baby, caring for a baby, or giving advice to new parents who seek it.
When prepared correctly in a safe, clean environment and given by caregivers who are educated in infant bottle-feeding, commercial formula is largely safe, nutritious, and (as originally intended) it can be a life-saving food. Thank goodness it exists because it can certainly help fix what’s broken! However, it also has the power to break what was never broken. Given that this website exists to help women who want to feed their children in the biologically natural way, educating about how formula use can break a breastfeeding relationship is unavoidable.
This information can help you understand the differences between what a mother’s body produces and what a factory produces. It matters because supplementary breastfeeding can be beneficial to an otherwise all-formula diet, but introducing supplementary formula to an otherwise all-breast milk diet does have a deleterious affect on various aspects of breastfeeding.
(In any case, feeding kids is always risky business no matter what you’re providing — Jessica from The Leaky Boob explains why you’re screwed no matter what here).
UNDER THE MICROSCOPE
Ever wondered what formula, cow’s milk, and human milk would look like if magnified 200x? Kelly Bonyata, IBCLC toyed around with her camera and took a shot for us. (Do any of you science-y folk have some observational feedback?)

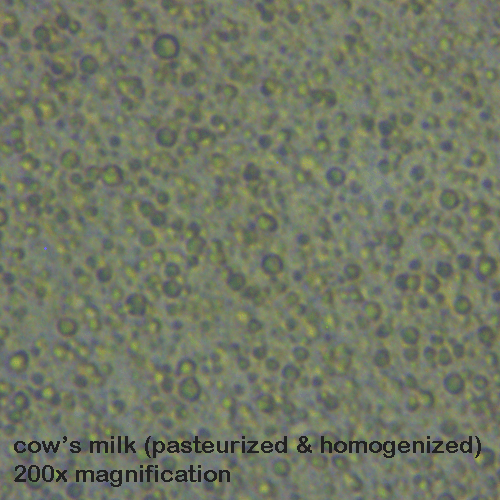

Moo Milk vs. Mom’s Milk
Cow’s milk is the breast milk of a species that needs its young to gain weight expeditiously and, secondarily, to develop a brain that has the capacity to understand life within the limits of a cud-chewing heifer. Human milk is designed to rapidly develop the brain first because it’s in the best interest of our species’ chance for survival; followed then by stable weight gain rather than a focus on rapid gain, which is not ideal for human babies.

YOU HEARD: “Your baby will stop gaining weight as quickly unless she switches to whole cow’s milk.”
TRUTH IS: The weight determining factors (proteins and fats) are very different in both types of milk and for very good reasons. While the percentage of fat in both milks is similar, human milk has high levels of brain-building ‘smart fats,’ while a cow’s milk is heavy with body-plumping saturated fats (DHA/ARA aren’t naturally present at all in cow’s milk!). Cow’s milk contains more than twice the amount of protein as human milk, and 80% of it is in the form of hard-to-digest casein, which is also linked to various diseases and allergies.
YOU HEARD: “Breast milk isn’t as nutritious for babies as whole cow’s milk after age one.”
TRUTH IS: A human infant’s natural development process does not suddenly stop when guests arrive for the child’s first birthday party. Calcium is four times higher in cow milk than human milk. Seems like that means it’s more nutritious, right? Well, maybe for a baby cow that needs to grow a much larger skeleton — and quickly. Even if you wanted your baby to receive a large dose of calcium, human milk is the better choice because calcium has higher bio-availability in mom’s milk than moo’s milk, which means a greater amount is actually absorbed. Iron is also more than two-thirds lower in cow milk than in human milk; this is an especially vital nutrient as babies run out of sufficient body stores of iron sometime during their first year.
Per The Vegetarian and Vegan Foundation:
“The high protein, sodium, potassium, phosphorus and chloride content of cow’s milk present what is called a high renal solute load; this means that the unabsorbed solutes from the diet must be excreted via the kidneys. This can place a strain on immature kidneys forcing them to draw water from the body thus increasing the risk of dehydration. The renal solute load of infants fed cow’s milk has been shown to be twice as high as that of formula fed infants (Martinez et al., 1985).”
YOU HEARD: “Whole cow’s milk is safer to drink than human breast milk.”
TRUTH IS: Safer for whom? A majority of the world’s population is lactose intolerant, meaning they cannot process lactose after weaning age. The ability to process this with the enzyme lactase in adulthood is actually a rather modern evolutionary trait. More than 90% of Asians, 65-70% of Africans, and interestingly only 10% of Caucasians are lactose intolerant.
Cow milk, the base of most formula, is both a common allergen for human babies and a well-documented intestinal irritant by nature (colic, anyone?). In fact, most health authorities recommend against introducing cow’s milk to an infant under the age of one — though many doctors often recommend that a child should switch to cow’s milk or as they call it “whole milk” (but breast milk IS “whole” milk!) at precisely one year.
Not to fear-monger about bovine dairy, but… there are many documented ill health effects associated with drinking cow milk at any age, including increased risk of acne, allergies, arthritis, various cancers, colic, constipation, coronary heart disease, Crohn’s disease, diabetes, dementia, ear infection, food poisoning, gallstones, kidney disease, lactose intolerance, migraine, multiple sclerosis, overweight/obesity, and osteoporosis. Early consumption of cow’s milk is a known cause of rectal bleeding in infancy, which can lead to iron loss and eventually anemia since cow’s milk is already low in iron itself.
If you knew about how today’s dairy cows live, you’d understand why their milk has become so unsavory. Being kept in close quarters in horrible conditions, many dairy farmed cows are riddled with infection and disease such as “brucellosis, bovine tuberculosis, foot and mouth disease, viral pneumonia and Johne’s disease” plus the breast infection mastitis, which affects about half of UK dairy cows.
A cow’s body responds to mastitis by “generating white blood cells (somatic cells) which migrate to the affected area in an effort to combat the infection. These cells, along with cellular debris and necrotic (dead) tissue, are a component of pus and are excreted into the milk” (Viva! Health). By the way, not all cows with mastitis show any physical symptoms of infection. That means they are left untreated and their milk makes it to the store shelf on time for parents to pick up this ‘toddler milk.’ Based on the amounts legally allowed in dairy products sold for human consumption, one teaspoon of cow’s milk can contain two million pus cells.
Basically…
“Milk from cows and goats is quite different in composition than human breast milk and, therefore, should not be fed to human infants.” – Physicians Committee for Responsible Medicine
Links:
- “Breastfeeding: Human Milk Versus Animal Milk” – NutritionMD
- “Calorie and fat content of various milks” – KellyMom
- “The Truth About Milk: Read” – Dave Rietz
- “When breastmilk turns to water and a cow makes better milk than you do” – Lakeshore Medical Breastfeeding Medicine Clinic
- “White Lies: A comparison between human milk and cow’s milk” – Viva! Health
- WhiteLies.org.uk

Via Messiah Mom
Modern Infant Formula vs. Human Milk
YOU WONDER: Just one bottle won’t hurt, right?
TRUTH IS: Introducing just ONE bottle of formula greatly alters gut flora (you’ve heard about the infant ‘virgin gut’?), to the point that it doesn’t return to normal for up to four weeks in an exclusively breastfed baby. If you don’t NEED to use formula, don’t. Find out why in this article by Marsha Walker, RN, IBCLC (reprinted by Dr. Jay Gordon). Also, find out what to do to restore gut health to your baby if you’ve already given formula, and better alternatives to formula supplements when you really just need a break from feeling like a human pacifier (you aren’t one though, okay?).
YOU WONDER: Isn’t DHA the same in human milk and formula?
TRUTH IS: DHA first accumulates in the infant brain prenatally during the last trimester of pregnancy, then the next natural source is mother’s breast milk. The essential fatty acid DHA was not first added to formulas in the United States until 2002. (Read more about DHA and other nutritional/medicinal goodies in human breast milk here).
Today, the DHA and ARA in infant formulas are patented and manufactured by one company, Martek Biosciences Corporation. This DHA comes from an oil called DHASCO that’s extracted from laboratory-grown algae using the toxic chemical hexane. Cornucopia Institute reports that only 40-50% of DHASCO is DHA, and the rest is foreign matter to a normal infant’s diet. Arachidonic acid (ARA) is also added to infant formulas to balance out the DHA; it’s made by extracting an oil called ARASCO from laboratory-grown soil with the help of, again, the toxic chemical hexane. The impure DHA and ARA oils in formula have not been thoroughly tested for safety, according to the Institute of Medicine, and the long-term effects have been seriously questioned (here is a review of the disturbing results of premarket safety tests).
YOU WONDER: Aren’t fats (lipids) the same in human milk and formula?
TRUTH IS: When newborns switch from liver glycogen to free fatty acids as an energy source at 24 hours after birth, they start requiring carnitine to transport it as they’re not physically mature enough to manufacture it on their own. Babies receive the carnitine they need naturally in breast milk, or added to formula if they are bottle-fed. However, a given formula may not include the ingredient carnitine, which often results in its infant consumers to “have impaired ability to use fatty acids and to regulate body heat and lipid levels” (Kacew).
The fats in formula usually derive from vegetable oils (corn, soybean, palm, and so on), many of which are genetically modified organisms (GMO) unless guaranteed otherwise (though some non-organic fatty oils have been added to and sold in organic formulas in flagrant violation of federal code). Find out where the fats in breast milk come from here.
YOU WONDER: Isn’t iron the same in human milk and formula?
TRUTH IS: The ingredients in formulas are typically present in much greater amounts than breast milk, not any indication that it’s superior or more vitamin-rich but that more of the same ingredients are absorbed in breast milk, therein less is needed. For example, formula has six times the amount of iron than breast milk. Parents who don’t understand about the difference in bio-availability between processed and naturally-occurring nutrients might believe that breast-fed babies would suffer at greater risk of anemia than their iron-overloaded, formula-fed peers. Find out in the Universal Vitamin Supplementation section of this post about why this is not true.
YOU WONDER: Isn’t cholesterol the same in human milk and formula?
TRUTH IS: Although cholesterol plays a vital role in building protective myelin sheaths around nerves and cognitive brain function, it’s present in formulas in only about one-third the amount found in breast milk. Milk cholesterol may help a child metabolize cholesterol better later in life.
YOU WONDER: Isn’t formula safer than human milk?
TRUTH IS: …safer for whom exactly? In developing nations, formula use has high rates of morbidity; it was estimated that one million babies died before their first birthdays per year in developing countries as a result of formula use. A recent study published in the medical journal The Lancet found that increased rates of breastfeeding could save 820,000 lives per year.
Consider that many families in poverty-stricken areas cannot afford formula so they must dilute it to make it last; sterile water for mixing and cleaning is scarce; children may have other medical problems worsened by not being breastfed; mothers may not have easy access to purchasing formula when needed; mothers may have trouble understanding formula labels and mixing instructions (Nestle’s international labels are written in English).
Let’s assume you live in a first world country and this doesn’t quite touch ‘close enough’ to home. You should be aware that in developed nations such as the U.S., there are other threats to family health that are raised by formula-feeding.

Va INFACT Canada, 2006
Here are a few other reasons why formula-feeding is still less safe than breastfeeding for you and your neighboring families in the Western hemisphere:
- Natural disasters. Who’s going to run out to the store for formula when mass flooding or a hurricane hits, hopefully making it home in one piece, mixing the formula in pitch-darkness when the lights go out, with no way to sterilize bottles or water — if you even have running water, that is?
- Emergencies. What if your car breaks down and you’re stranded on the side of a scarcely-traveled road? How will you safely mix your formula? What if you forgot your formula, bottles and other feeding apparatus at home? What if your flight gets delayed on the runway for hours and you only brought enough formula to last the expected travel time? If a tragedy befalls a nursing mother, her baby can always switch to formula; switching from formula to breast… well, that’s quite a mountain to climb, and sometimes an impassable one.
- Digested formula can be toxic to cells in young babies. This study was described here to show that “digestion of formula led to cellular death, or cytotoxicity – in less than 5 minutes in some cases – while breast milk did not,” which contributes to the second-highest killer of premature babies, the condition called Necrotizing Enterocolitis.
- Contaminants, genetically modified organisms (GMOs), beetle parts/larvae, and bisphenol-A (BPA). See more on toxins in infant formula and breast milk here.
- A breastfeeding mother is virtually always present. If a mother formula-feeds so she can return to work, her salary can realistically cover the cost of at least a year’s worth of formula, plus the cost of childcare. And of course, it will cost her the fortune of being with her baby. A formula-fed baby is much more likely to die from SIDS, for example, in part because breastfed babies are kept close to the mother at night and can be attended to more quickly should any medical intervention be needed. Also, if a breastfeeding mother falls ill with a virus such as swine flu, continuing to nurse is the best protection she can give her baby. Because formula doesn’t offer anti-virus agents, an infected non-breastfeeding mother might be encouraged to separate from her baby.
- Safety regulations. “The FDA does not approve infant formulas before they can be marketed. All formulas marketed in the United States, however, must meet Federal nutrient requirements.” – US Dept. of Health & Human Services. Guess who regulates the safety of breast milk? It’s entirely up to the mothers who produce it.
- Hygiene. Bottles require constant sterilizing and impeccable cleaning (towel-dry ain’t gonna do). By contrast, normal breasts actually should not be cleaned prior to nursing. This is an issue of bad bacteria vs. good bacteria. Typically, you can’t just whip out a bottle of formula when baby gets fussy like you can with a breast (though it is a bit weird hearing “that mom just whipped it out in public!” like she was seen furiously making sundaes…). Breast milk is made while mom sleeps, while she sits on the couch, while she drives, and so on — and she doesn’t need to wash her hands, boil water, sterilize her nipples and scrub her breasts, then feed, and wash, rinse and repeat.
YOU WONDER: Wait…is anything the same in human milk and formula?!
TRUTH IS: Sure! Well, they are both infant foods. Go ahead, check out this poster from BC-Baby Friendly Network and decide for yourself how similar they really are: “Did you ever wonder what’s in breast milk and formula?”
Toxins in Infant Formula
Just because formula is literally formulated (in a lab and then by a manufacturing company) doesn’t mean it’s ‘perfect.’ Powdered formula is never sterile even if prepared with boiled water because it must be newly prepared, and proper mixing techniques aren’t always followed or in some cases never learned.
Sometimes contamination occurs during the manufacturing process, as has been the case with the Enterobacter sakazakii outbreaks in which 20-50% of affected infant formula consumers died.
Read my list of FORMULA RECALLS (not a complete list).
Breast milk has also been found to contain environmental toxins, which you can read more about here.
WHAT’S THE MYSTERY IN MAN-MADE MILK?
- Hidden toxins in baby formula;
- Arsenic found in “organic” baby formula at 6x higher levels than the USEPA safe drinking water limit;
- Polycyclic aromatic hydrocarbons (chemical pollutants) were found in highest levels in infant formula than in commercial cow milk and human milk;
- Pthalates in formula;
- Melamine in formula 2008 scandal; here too
- Rocket fuel additive perchlorate in two of the biggest formula companies’ products;
- Formulas contain 100 times more of the food toxin called Advanced Glycation End Products than breast milk
- Inorganic components included in formula labeled as “organic” formulas
- Beetle parts in Similac formula
- GMOs – Genetically modified corn, soy, and sugar beets are present in many of the top three formula companies’ products (these three companies represent 90% of the market). The names: Similac (Abbott), Enfamil (Mead Johnson), and Gerber (Nestle). Genetically modified maternal goodness is in breast milk. The names: Mom, Mama, Mommy, Mother, Maman… A pediatrician discusses the what GMOs in formula means for infants here. Have you considered making your own infant formula at home to avoid GMOs?
- Bisphenol-A (BPA) in the linings of formula containers – BPA has been detected in breast milk too, but levels can be reversed by cleaning up a nursing mother’s diet and environment. BPA in formula canisters is just simply… there. In 2010, the European Food Safety Authority said that liquid formula packaging contains significant amounts of BPA (the risk is much lower with powdered formulas): “Infants fed with liquid formula are among the most exposed, and those fed formula from polycarbonate bottles can consume up to 13 micrograms of bisphenol A per kg of body weight per day.” BPA has been linked to various cancers, urogenital abnormalities, lower semen quality, ADHD, and prostate problems in boys; and premature puberty and breast cancer in girls. It’s also been observed as a causal factor in obesity, permanent changes in the genital tract, type 2 diabetes, and much more. Thankfully, in 2013 the FDA banned the use of BPA in formula containers (it was previously banned in children’s products in China, the European Union, Canada, and 11 U.S. states). However, one formula manufacturer insisted it has no specific plans to use BPA in its packaging but “reserves the right to do so in the future should circumstances warrant it.” (Uh, does that sound convincing to you?) Surely, organic formulas don’t have this cancer-causing chemical in their packaging obviously… right? Not quite. Labeling still remains unclear enough that we can’t be sure what’s replacing the supposedly absent BPA, and even organic brand formulas have been found to contain this hormone-disrupting chemical.



